(Disclaimer: This article was originally written Sunday, December 6, 2020. In this published version, the names of nine of the ten mothers have been removed to protect their anonymity.)
Nassau, Bahamas – Loud, agonizing cries that once bounced off the four walls of the small and lonely labor ward at Princess Margaret Hospital (PMH), in Nassau, Bahamas, are now reverberating outside the facility and onto the eyes and ears of the public.
Expectant mothers of all ages who enter through these doors with the hope of having a safe and healthy delivery, are taking to social platforms and traditional media outlets to tell what some have described as “nightmares”. What should be a moment of love, joy, and bonding between mother and child is instead a fight for survival.
For 20-year-old Shakinah Dean and 36-year-old Zennrine Ramdas, this fight became a reality, as both succumbed after giving birth just two weeks apart, joining the country’s most recent pool of maternal death cases during the COVID-19 pandemic.
“Doctors contacted me once before she passed, then [once] after she passed away,” said Karen Dean about her daughter Shakinah, who died on August 20. “They spoke to the type of treatment they [were] giving her and what treatment they would use if it doesn’t work.”
Karen told The Click that doctors took over one week to inform her of the cause of her daughter’s death, which they determined was the result of COVID-19. However, three months later, the mother is still not satisfied with that conclusion.
“I think if PMH had taken better care of her, she would’ve still been here today,” she said of her daughter who left behind a healthy baby boy.
In an earlier interview with The Nassau Guardian, Karen explained how due to COVID-19 restrictions, her only line of communication with her daughter during her final moments was through cell phone.
“Shakinah has never had a situation that I was not physically present to assist her [with]. If I was able to or thought that she was dying, I would put my life on the line to be there with her,” she told The Click. “It was the most difficult thing in my life.”
It would be just 15 days later, on September 4, that Ramdas, an otherwise healthy mother of seven, would also pass away at PMH after giving birth to a healthy baby girl.
In an interview with The Nassau Guardian, one of Ramdas’ older daughters, Dwiesha Berry, described how her mother’s health deteriorated over just a few days after having been discharged, noting that she “could barely move”.
According to Ramdas’ mother, Veronica Ramdas, doctors calculated that Ramdas, who had to be readmitted, died of a womb infection. However, the origin could not be determined.
“It’s not a regular occurrence on a maternity ward,” said Nurse Cleola Hamilton, former president of the Bahamas Nurses Union (BNU). “It’s also a traumatic experience, especially if a normal birth is anticipated.”
Hamilton, who was a founding member of the BNU in 1999 and served as its president until 2013, noted a few possibilities that could lead to an abnormal birthing experience.
“There are a number of causes and each case is at its merit,” she explained. “Through negligence, underlying problems or unforeseen circumstances, each case has to be examined.”
Key findings from data published by the Centers for Disease Control from 14 U.S. Maternal Mortality Review Committees between 2008 and 2017 corroborate Hamilton’s expertise.
The data concludes that maternal death is the result of either pregnancy-associated complications, which is death from a cause that is not related to pregnancy, such as pre-existing conditions; pregnancy-related complications, which is death from an unforeseen/underlying condition that the pregnancy manifested or exacerbated; or death that is deemed preventable, which speaks more to the conditions of and within the facility, available resources and how timely assistance is rendered, among other factors.
Both deaths came as a shock to the public, as Dean and Ramdas were young and healthy. Although, there are instances where maternal death, unfortunately, cannot be avoided, even with the best care, especially now during the COVID-19 pandemic.
Amid these controversial deaths, data showing maternal death and live birth ratios at PMH, and interviews with nurses, government officials and the many mothers who took to social media to recount their own experiences and apprehension, all show how women are being met with poor and even potentially dangerous conditions upon their arrival to give birth.
According to maternal death figures obtained from the Department of Statistics, there have been 79 recorded maternal deaths at the facility, over a 43-year span, between 1971 and 2014, with most deaths, 10, having occurred in 2001. That is an average of 2.5-3 deaths per year.
Although the Public Hospitals Authority (PHA), which is the governing body for all public health institutions in The Bahamas, reserves the right to withhold patient confidentiality, PHA Director of Communications Judy Terrell noted in both Dean’s and Ramdas’ news stories, and to The Click, that both deaths are under investigation.
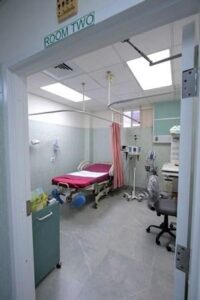
The newly renovated Princess Margaret Hospital Maternal and Child Health Labour Unit, Maternity Ward, on Tuesday, August 7, 2018. (BIS Photos/Derek Smith)
It was the story of Kayla Edwards-Dean, a 35-year-old, who lost twin boys during childbirth, in August 2020, that set social media ablaze. After resonating with Dean’s story, Edwards-Dean thought it necessary to share a thorough account of her ordeal at PMH, which opened the gates for hundreds of other women to share their own ill-fated experiences.
The ten mothers who reached out to The Click, in response to a Facebook post in a secret group for moms, all claim to have been greeted by either overcrowded hallways, insufficient beds, unsanitary bathrooms, a dilapidated recovery room, and careless doctors and insulting and dismissive midwives and nurses, or a combination of all.
Such was the case for a mother of two, who reached out with tales of alleged carelessness by her doctor and midwife during both of her children’s births.
“My son weighed nine pounds. I almost lost my life because I pushed him via vaginal birth, not knowing that he was too big for me to push,” she recalled. “The midwife snipped me with scissors or whatever it was, just to help me, after not knowing that I couldn’t really push because of his size. I told her [but] she didn’t believe me. I got 15 stitches and the doctor [sewed] gauze inside me. I found out 15 days later, after smelling [an] awful smell come out of me. The doctor said If I [had] waited two more days, I would’ve died, due to an infection.”
The 31-year-old, who almost fell victim to the same fate as Ramdas, shared a second story of the birth of her daughter two years after.
She revealed that during this birth, in 2012, she had to have an episiotomy, an incision in the perineum during childbirth to facilitate delivery.
“After my daughter came out, the placenta didn’t come out, so the nurse decided to pull it out and [that] caused a hemorrhage,” she explained. “I had to get two IV drips and had [a] pill inserted in my anus to stop the bleeding. I was hospitalized for five days to try [to] stop the bleeding.”
Saddened by all the mothers who did not make it out alive, this mom strongly believes that a lack of professionalism and training almost ended her life, twice. However, her account of alleged carelessness is only one of many.
A second mom, who gave birth in October 2017, thought her delivery would be smooth sailing. With no labor pains or contractions, things seemed to have started on the right track. However, according to her, “the worst” did not begin until after she delivered her baby.
“I’m not sure of the [nurse’s] name who stitched me up, but I was able to get a video of her. She [left] gauze in me (after a vaginal birth) after she stitched me up,” she explained. “When I went home after my two-day stay at the hospital, I noticed I wasn’t bleeding as much as I thought I should and the little that was coming out was very dark and smelled horrible. It wasn’t until my mom started to get worried about it, [that she] decided to take me to the hospital.”
She explained that upon arriving at the hospital, a doctor examined her and discovered the gauze that was left inside of her. She noted how the doctor thought it apt to tear through her stitches to pull the gauze out.
“I was screaming and crying, pleading for him to let me be because I couldn’t take all of that unbearable pain,” said the 21-year-old.
She also mentioned how a janitor, who was just outside her room, declined to clean the room after she was done, because to her, “In there [smelled] like a dog died inside her [the patient].”
The mother of one also allegedly contracted an infection and had to remain hospitalized for two more days without having her newborn by her side. She mentioned to The Click that aside from the physical pain she endured, what hurt her the most was that she was never issued an apology.
Although current Minister of Health Renward Wells sympathizes with the death of mothers and emerging stories of their alleged mistreatment at PMH, as is stated in this September 8 interview, he also noted that “the medical community, both public and private, is stretched,” and that patients do not file official complaints.
This was the case for a fellow registered nurse, who considered filing a complaint but became discouraged after realizing how arduous the process would be.
“My labor experience was horrible and left a scar, where I didn’t even want to have any more children,” she told The Click. “I was told to write a letter but being a nurse in the system, I know what it is to be victimized, especially by a service I will need again in the future.”
Also responding to the Facebook post, she recalled her October 2015 ordeal at PMH.
“I was harassed by the clerk while in labor for an admission fee that I repeatedly advised her I didn’t have at the moment; all because I was a ‘private patient,’” she explained. “The midwives at the desk laughed at me when I told them my contractions were five minutes apart. Being a first-time mother, I told them based on the app I was using, that’s what I got; and when I was checked, it was correct.”
She went on to describe how she was denied painkillers for intense back pain from when she arrived at 8 a.m., “until the shift changed after 3 p.m.,” seven hours later; also recalling that one of the “foreign” midwives allegedly threatened to “put a probe internally” on her baby’s head if she did not keep still and lie on her back, despite her cry that it felt like her back was being ripped apart.
Despite this moment of difficulty, the mother of two did acknowledge that the morning shift nurses, midwives and doctors were pleasant and checked on her quite often.
The 33-year-old also described being “chastised for co-sleeping”, although, according to her, there was no other option, as the bed had no rails and could not roll up. Throughout her experience, she was reportedly not given any information about her delivery, her baby, or anything that transpired. The healthcare workers allegedly forced her to walk to her vehicle, instead of being transported via wheelchair. One of the most unusual circumstances she recalls is her husband not being allowed to hold their daughter while leaving the ward, as it was hospital “policy”.
Similar to the second mom who spoke to The Click, the expectant nurse admitted that her biggest issues were, “Mainly, the attitude and treatment by the midwife on the evening shift,” and recalling while she was in labor that she was “forgotten in the staff room and not given any updates”, while also having to share the “nasty, bloody bathroom with other patients”.
“I don’t know who is responsible for cleaning, but they need to do a better job,” she added. “The women also need to take more pride in how they leave the facilities because some are just nasty.”
When asked if nurses were aware that she was a fellow nurse, she replied, “They knew. Plus, I was in the staff room that’s on [the] antenatal ward. It just didn’t make a difference.”
In response to the criticism nurses and midwives receive, one midwife, who wished to remain anonymous said, “It hurts.”
“Nobody is perfect. Our outcomes are more positive than negative, but Bahamians have a high sense of entitlement and expectations and it’s very upsetting when they generalize,” she shared. “Sometimes, due to a high demand in work, things get missed unintentionally. A doctor or nurse can get caught up and not have the time to explain the details of everything, but we do our best to inform [the patient].”
She added, “We are professionals. We’re not at liberty to explain a lot of things to the public, but we still must follow certain protocols, rules and guidelines. Also, our institution doesn’t safeguard us, so, in some ways, we have to take the fault. It’s easy to blame us because we’re the face. They see us more than everyone else.”
A second midwife, who also wished to remain anonymous, concurred.
“Remember, during any form of communication, things can be misunderstood, on either the receiver’s or the sender’s end, especially when you have a concerned mother or family member,” she explained. “Sometimes, things on both ends can be misunderstood and an attitude is perceived. Midwifery is a high-stress job because on a regular day, you have two lives in your hands.”
Despite her below-par experience as a patient, the nurse empathizes with the midwives as a fellow healthcare worker within the public health system.
“Honestly, there are only the same few bad apples, but because nobody says anything, they all tend to fall in the same boat,” she explained.
“Bedside nursing skills are lacking in the profession now. I remember the joy and excitement I had as a new nurse 12 years ago. The frustration of dealing with the system, management, facilities and all the other issues tend to change you, if you allow it. Then again, some just never had it in them to begin with.”
In agreement is a fellow nurse who also requested anonymity.
“I feel that with the stories that emerge, you have the good with the bad, so everyone’s experience will differ,” she explained. “I also feel that the competent authorities are aware of the problems that plague the medical field, but they always turn a blind eye, as priorities are placed on the wrong things.
In addition to the expectant nurse, two other women, among the ten who reached out to The Click, agreed that nurses and midwives are not always to blame.

This photo taken by a mother of one shows apparent hazardous conditions to which mothers and their newborns are exposed once transferred into recovery at PMH. (Anonymous)
“If the conditions [were] better, the nurse[s] would work better. I feel like they are overworked and underpaid, need to rest and need a better [working] environment,” said a 27-year-old woman who recently gave birth at PMH.
She also mentioned that her “nightmare” started once she was transferred over to the recovery unit, citing a leaking roof, a nasty bathroom and the facility’s overall need for major renovations.
“I always tell patients who complain about there not being any hot water or that there are spills or blood stains in the bathrooms to write a letter to administration or to the minister of health, because as a nurse, there is nothing more I can do. The women are able to clean up after themselves,” said the first midwife.
On the contrary, a 29-year-old mom sang a nurse’s praises whom she said was like “an angel” in the delivery room.
“On August 24, 2016, I went into labor with my second son. I felt like I had everything under control seeing that my first son wasn’t so bad, but it was totally different,” she told The Click. “The contractions [were] so bad, I couldn’t lay on my back and I was told I had to, in order to push. It was so bad that I just laid there and was ready to give up on my life, on my [baby’s] life. I kept telling the nurse I can’t push.”
She explained that there was a janitor cleaning around her who asked, “If you don’t push, who will push for you?” but that, luckily, the nurse’s words, “You didn’t come this far to give up. Let go. Push!” rang truer.
“It felt like it was the devil and an angel in the room, literally,” said the mother of two. “Because of that nurse, I strongly believe it’s the reason why my son and I made it out that room alive, just because she encouraged me to push. If I paid any mind to that other lady [the janitor], I would’ve just laid there.”
===
Another 29-year-old expectant mothers, who endured a Caesarean section (C-section) back in 2010, believed that she was the victim of negligence.
“I’m allergic to many medications and when I woke, I was gasping for air and my face was swollen,” she recalled. “As they flushed my system, I looked down at my wrist and the tag with my medicine allergies was gone.”
This mom explained that when she questioned why her tag had been removed, nurses told her that it “got bloody” during surgery.
“It baffled me that they didn’t care to replace it. So, the nurses didn’t know not to give me the medications. It could have killed me!” The mother of one, whose daughter is now 10, said this experience has left her in fear of having another child.
Sharing this fear is a 24-year-old and 34-year-old Kenderia Cargill.
“My daughter is five, but I’m pregnant now and I’m terrified,” the 24-year-old mom told The Click. “I don’t ever want to go back on that public ward to have another child.”
Cargill, who was nearing her due date in this September 11 interview, also expressed apprehension toward giving birth at PMH.
“If I had the money, I would go somewhere else to do it, but PMH is the only place right now,” she shared. “Even before COVID-19, the hospital was not in a good state. So, hearing all of the stories now, it’s believable. Once one story comes out, everything comes out. I just hope it’s an in-an-out situation for me.”
In response to the 24-year-old mother’s less-than-favorable view of the nurses’ attitudes, the nurse admitted, “A lot of the times, nurses do have a bad attitude, but I don’t know where it stems from. It could be individuals bringing home to work, or just being miserable.”
However, she told The Click that, despite what is happening around her, she loves her field of work but wants those in charge to make the necessary changes.
“As a nurse, I have learned to adjust and make do with what is there because fretting oneself can make me less competent at my job and cause problems to arise for me when dealing with a patient. I love my job and have seen the good, bad and ugly and nothing is perfect, but I wish more could be done to fix these issues, since one’s health should be a priority.”
===
Statistics that list the total number of live teenage births between 1986 and 2014, reveal that the highest number of births, 34, occurred in 1993, in the 10-14 age group, with the lowest number, one, occurring in 2014. These results also reveal that the highest number of births, 1,001, occurred in 1992, in the 15-19 age group, with the lowest number, 425, occurring in 2014.
This decrease can be attributed to the establishment of the Ministry of Health’s National Family Planning Policy, in 1995, which led to over 10,000 postnatal teenage mothers requesting and using contraceptives.
Despite this downward trend, a mom, who gave birth two years ago at the age of 16, said nurses treated her like she was nothing more than a statistic.
“They talked to you like you were nobody,” said the mother of one. “They (nurses) [left] me in the blood from 4:04 p.m. until after 8 p.m. They let me bathe at 10 p.m. and I didn’t see my baby until 1 a.m. The nurses [were] saying I have to wait [because] they don’t have beds, [and] the food was cold.”
The second midwife revealed that, as recently as two years ago, midwives have been welcomed into the delivery room, specifically for teenage pregnancy cases, to ensure a tolerable experience.
“People listen to bad news more than good,” she said. “I’ve worked with adolescent mothers for the last two years and I’ve had the opportunity to go on the ward with them and be there as an added comfort and familiar face.”
Although the now-18-year-old maintains that “PMH is the worst place to give birth”, she did admit that she had “nice midwives but the nurses are the trouble”.
Despite the numerous allegations by expectant mothers, current BNU President Amancha Williams could not be reached for comment.
However, while turmoil increased on the labor ward at PMH, so did it at other healthcare facilities on the island, such as Sandilands Rehabilitation Centre (SRC), where it was reported on August 20 that “more than a dozen” nurses called in sick after “experiencing symptoms”.
“The difference between now and pre-COVID is the screening,” the first midwife explained. “Women 20-plus weeks pregnant [are] given a questionnaire to complete, asking about symptoms such as cold, cough, fever and their travel history or contact with COVID patients. In addition, only two people are allowed inside the ward’s waiting area to comply with social distancing.”
Just a little under one month later, Williams, who “was concerned about the safety of the nurses,” was met with an additional 200+ nurses at PMH, SRC and the Rand Memorial Hospital who called in sick on October 14, “Amid growing tension over working conditions and a new shift system”, Eyewitness News reported.
“Patients that are COVID-positive were initially nursed in isolation on [the] private surgical ward but now the original antenatal ward is being used for COVID patients,” the first midwife explained. “We can’t turn anyone away.”
This is not new for PMH.
Data obtained by the Department of Statistics conclude that a yearly average of 3,988 live births occurred at PMH, between 1993 and 2016, with the highest number, 4,908, occurring in 1993. When calculated, this equates to approximately 409 births per month, which is about 13 births per day.
While an average of 13 births may seem low, especially in 1993, when the island’s population was just 172,196, as is seen in Table 1.6 of the New Providence Census Report of 2010, it is twice the amount of beds that is available, today, based on the first midwife’s calculations.
Now, with an island population of 220,000-plus, the midwife explained that only 14 beds can fit in the antenatal unit, 17 beds in the postnatal unit and 12 beds on the obstetrics & gynecology ward, which is a total of 43 beds. The midwife also noted that, despite these 43 beds, it is standard policy for expectant mothers to give birth in the ward’s six designated laboring beds only, unless there is a rare occasion that prevents them from doing so.
In such a case, where the ratio of beds to expectant mothers is disproportionate, there may be no choice but for childbirth to ensue in the hallways; an ordeal a mother of one allegedly endured nine years ago.
This was also the experience for first-time mother Celeste Sweeting.
“The hospital, itself, needs more space, needs to be revamped, needs to be totally redone,” Sweeting told The Click. “The ward is always full. When I was admitted in August 2016 to have my daughter, I was told I needed a C-section, but the theater was full, so that didn’t happen. I just was hooked up to more machines and left alone.”
In 2018, Sweeting, then-25, started an online petition, after reading one too many childbirth horror stories on social media, with the hope that it would grab the attention of then-Minister of Health Dr. Duane Sands – which it did.
“Why should we have mothers in a small, congested clinic with sick people; their young babies, one and two months old, in the same building with sick people who aren’t even diagnosed yet? It just doesn’t make any sense,” said Sweeting. “You all are already begging for space in the hospital, so put mothers elsewhere and you all can have the entire ward.”
Based on this 2017 article published on the PHA’s website, Prime Minister Dr. Hubert Minnis, who is a doctor of obstetrics and gynecology, seemed to agree.
While on a tour of the facility, shortly after being elected prime minister in May 2017, Dr. Minnis “promised the country and staff at the Princess Margaret Hospital a new maternity wing”. However, what was promised to be a “wing”, turned out to be minor renovations.
One year and three months later, in August 2018, the delivery unit, which “used to be gloomy and dark”, was given a “long overdue facelift” with new flooring and “bright” new paint, according to this 2018 article published on the PHA’s website. This undertaking was completed through a partnership between the former Minister of Health Dr. Sands, a practicing cardiothoracic surgeon, and a local OBGYN, Dr. Leon Dupuch.
The article also mentions that 25 beds were added to the maternity ward, with the hope that it would finally allow for one bed per room, affording mothers the privacy that allows a partner or loved ones in the room during childbirth. However, with the pandemic commanding space and attention, these very beds, and more, are occupied by COVID-19-positive and COVID-19-suspected patients, leaving even less available to expectant mothers.
===
Princess Margaret Hospital, with its mission: “To provide affordable, holistic, quality healthcare appropriate to the needs of our clients by a team of committed, caring professionals striving through a research-driven environment,” was commissioned in 1953 as The Bahamas’ premier, acute tertiary facility.
Sixty-seven years later, in 2020, stories of alleged malpractice and unaccommodating spaces exist, and in growing numbers.
Walls of the maternity ward have been replaced with the walls on social media, which have become digital diaries and journals of justice for mothers who can no longer stand to remain quiet.
The institution boasts having treated over two million emergency patients, logged over 250,000 surgical operations and registered over 200,00 births in its Maternity Unit.
Yet, even with these numbers, mothers such as Edwards-Dean, Cargill, Sweeting and countless others are still in fear of giving birth again; and mothers-to-be, after getting wind of all the horror stories, are following suit.
Still, it is the hope that with more investigations and mothers and advocates speaking out, that much-needed improvements will be made to the country’s largest, most affordable, and accessible healthcare facility, sooner than later.

